
manual resuscitator
Manual Resuscitators: A Comprehensive Overview
Manual resuscitators, vital in emergency medicine, deliver breaths when spontaneous ventilation is inadequate, offering a lifeline during critical resuscitation scenarios.
Manual resuscitators, frequently termed bag-valve-mask (BVM) units, represent a cornerstone of emergency airway management. These devices provide positive pressure ventilation, crucial when a patient cannot maintain adequate respiratory effort independently. Their simplicity and portability make them indispensable tools for pre-hospital care, emergency departments, and operating rooms.
Effective utilization demands a thorough understanding of proper technique, as both under- and over-ventilation can lead to detrimental consequences. Recent studies highlight the difficulty in consistently achieving recommended tidal volumes during resuscitation, often resulting in excessive ventilation. Consequently, guidelines now advocate for volume-restricted bags, particularly for adult patients, and the incorporation of Positive End-Expiratory Pressure (PEEP) to improve outcomes and minimize lung injury.
What is a Manual Resuscitator (Bag-Valve-Mask)?
A manual resuscitator, commonly known as a bag-valve-mask (BVM), is a handheld device used to provide artificial ventilation to patients who are unable to breathe adequately on their own. It consists of a reservoir bag, a one-way valve system, and a mask that creates a seal over the patient’s mouth and nose, or connects to an endotracheal tube via a 15mm or 22mm fitting.
The bag stores oxygen, while the valve system ensures airflow travels in only one direction – from the oxygen source to the patient. Squeezing the bag delivers pressurized air into the lungs. Modern resuscitators can be gas-powered, delivering 100% oxygen with reduced user exertion, though these are generally recommended for adult patients, not infants or small children.
Historical Development of Manual Ventilation
The evolution of manual ventilation began with mouth-to-mouth resuscitation, practiced for centuries. Early 20th-century advancements saw the introduction of mechanical ventilators, bulky and requiring significant infrastructure. However, the need for a portable, readily available ventilation method spurred development of the bag-valve-mask (BVM).

The BVM emerged in the mid-20th century, offering a simpler, more accessible alternative. Initial designs focused on basic functionality, gradually incorporating improvements in materials, valve systems, and mask designs. Contemporary advancements include volume-restricted bags, aiming to prevent overventilation and reduce the risk of manual-ventilation-induced lung injury (MVILI). Current guidelines, like the 2021 NAEMSP position statement, emphasize optimized techniques and the use of PEEP to improve patient outcomes.

Types of Manual Resuscitators
Manual resuscitators vary by patient age – adult, pediatric, and infant – and include gas-powered options offering higher oxygen delivery capabilities.
Adult Manual Resuscitators
Adult manual resuscitators are designed for patients presenting with respiratory failure or arrest, requiring immediate ventilatory support. These devices typically feature larger reservoir bags, capable of delivering higher tidal volumes necessary for effective lung inflation in adults. Current recommendations, stemming from a 2021 NAEMSP position statement, increasingly advocate for the utilization of volume-restricted bags even for adult patients.
This shift aims to mitigate the risks associated with overventilation, a common complication during manual ventilation that can lead to hemodynamic instability and potential lung injury. While traditional adult bags deliver substantial volumes, employing pediatric-sized bags can help clinicians adhere to recommended tidal volume targets. Gas-powered resuscitators are also considered superior for adult use, providing consistent oxygen delivery and reducing rescuer fatigue, though they are not recommended for infants or small children.
Pediatric Manual Resuscitators
Pediatric manual resuscitators are specifically engineered for infants and children, differing significantly from adult models in reservoir bag size and mask configurations. These devices deliver smaller tidal volumes appropriate for the smaller lung capacities of pediatric patients, preventing overinflation and potential lung injury. Careful selection of the correct mask size is crucial to ensure an effective seal and optimal ventilation.
While gas-powered resuscitators excel in adult resuscitation, they are generally not recommended for infants or small children due to the risk of delivering excessive pressures. The NAEMSP guidelines emphasize the application of Positive End-Expiratory Pressure (PEEP) in both adult and pediatric patients to improve oxygenation and lung recruitment. Maintaining appropriate ventilation targets during pediatric resuscitation can be challenging, highlighting the need for ongoing training and adherence to established protocols.
Infant Manual Resuscitators
Infant manual resuscitators represent a critical component in neonatal and pediatric emergency care, demanding precise application due to the unique physiological characteristics of newborns. These devices feature the smallest reservoir bag volumes and correspondingly sized masks, meticulously designed to deliver safe and effective ventilation to the smallest patients.
Unlike adult resuscitation where gas-powered options are favored for consistent oxygen delivery, infant resuscitation relies heavily on skilled manual technique. Overventilation poses a significant risk, potentially leading to lung injury; therefore, utilizing volume-restricted bags is increasingly recommended. Achieving optimal ventilation requires careful monitoring and adherence to guidelines, ensuring appropriate tidal volumes and, when indicated, the application of PEEP to support oxygenation and minimize lung damage.
Gas-Powered Resuscitators vs. Manual Resuscitators
Gas-powered resuscitators offer distinct advantages over traditional manual resuscitators, primarily in their ability to deliver 100% oxygen consistently and reduce rescuer fatigue. They require minimal exertion for ventilation, a crucial benefit during prolonged resuscitation efforts. However, their application is generally recommended for adult patients, as they are not ideally suited for infants or small children due to potential over-inflation risks.
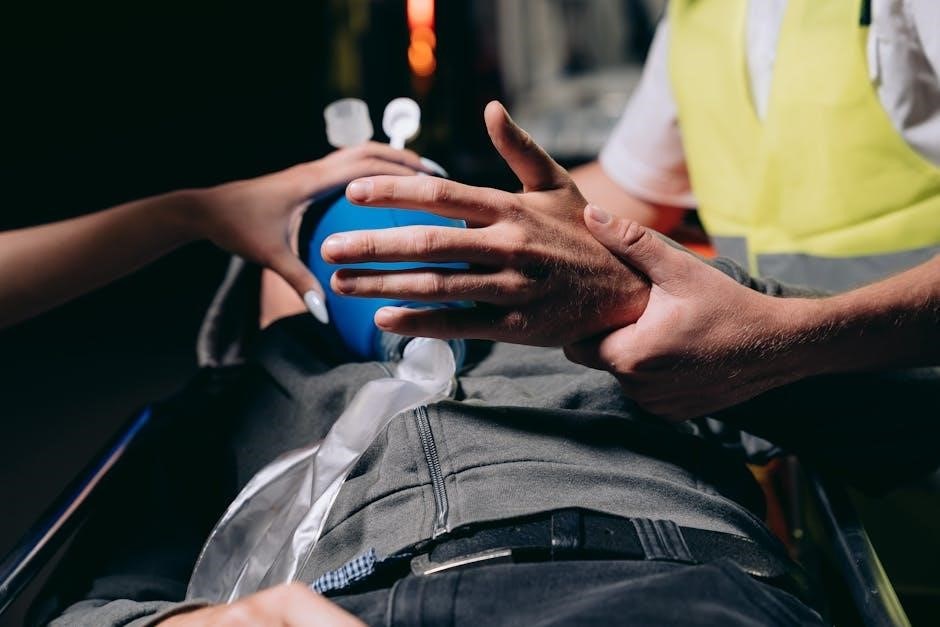
Manual resuscitators, while requiring rescuer effort, remain essential, particularly in pediatric settings. They connect to standard 15 and 22 mm fittings for masks and tubes. The choice depends on the clinical scenario; gas-powered devices excel in sustained ventilation, while manual devices offer portability and versatility, especially when oxygen source limitations exist.
Components of a Manual Resuscitator
Essential components include the reservoir bag, a crucial valve system ensuring unidirectional airflow, and adaptable masks with 15mm or 22mm connectors.
Reservoir Bag
The reservoir bag is a fundamental component of a manual resuscitator, serving as the primary storage for oxygen before delivery to the patient. Typically constructed from latex or silicone, its volume is carefully calibrated to provide adequate tidal volume – the amount of air delivered with each breath. Maintaining a fully inflated reservoir bag is crucial; collapse indicates insufficient oxygen supply and can lead to the delivery of rebreathed carbon dioxide.
Different bag sizes correspond to patient populations, ensuring appropriate ventilation. The bag’s elasticity and responsiveness directly impact the ease of ventilation for the rescuer. Regular inspection for leaks or deterioration is vital to ensure optimal performance. Proper bag maintenance and replacement are essential for consistent and effective manual resuscitation, directly influencing patient outcomes during critical care scenarios.
Valve System (One-Way Valves)
The valve system, incorporating one-way valves, is integral to the functionality of a manual resuscitator, ensuring unidirectional airflow. These valves prevent the backflow of exhaled gases from the patient back into the reservoir bag, and also prevent ambient air from entering the system during bag inflation. This precise control is vital for delivering high-concentration oxygen and avoiding rebreathing of carbon dioxide.
Typically, two one-way valves are present: an inlet valve allowing oxygen entry and an outlet valve directing air to the patient. Regular inspection of these valves for proper sealing and function is paramount. Damaged or malfunctioning valves compromise ventilation effectiveness and patient safety. Maintaining the integrity of the valve system is crucial for delivering consistent, safe, and effective manual respiratory support during resuscitation efforts.
Masks and Connectors (15mm & 22mm Fittings)
Manual resuscitators utilize masks and connectors with standardized fittings – primarily 15mm and 22mm – to interface with both the device and the patient’s airway. These connectors ensure a secure and leak-proof connection to face masks or endotracheal tubes. The 15mm fitting is commonly found on pediatric equipment, while the 22mm fitting is standard for adult applications, though both sizes can be adaptable depending on the clinical scenario.
Proper mask selection is crucial for effective ventilation, ensuring a tight seal to minimize air leakage. Different mask designs cater to various patient anatomies and resuscitation needs. Compatibility with standard oxygen delivery systems is also essential, allowing for supplemental oxygen administration. Maintaining a readily available supply of appropriately sized masks and connectors is vital for efficient emergency response.

Proper Usage and Technique
Effective manual ventilation demands correct hand placement, a consistent squeeze rate, and supplemental oxygen to deliver optimal breaths and support patient oxygenation.
Correct Hand Placement and Squeeze Technique
Achieving effective ventilation with a manual resuscitator relies heavily on proper technique. The “C-E” grip is commonly taught: the thumb and index finger form a “C” around the mask, while the remaining fingers form an “E” supporting the jaw. This ensures a tight seal.
Squeeze the bag smoothly and deliberately, avoiding excessive force or rapid compressions. Aim for a rate of 10-12 breaths per minute for adults, and adjust accordingly for pediatric patients. Observe for visible chest rise with each breath, indicating adequate ventilation. Avoid overventilation, as it can lead to complications like manual-ventilation-induced lung injury (MVILI).
Consistent hand placement and a controlled squeeze are crucial for delivering appropriate tidal volumes and maintaining effective oxygenation during resuscitation efforts. Proper training and regular practice are essential for mastering this vital skill.
Achieving Effective Ventilation
Effective ventilation with a manual resuscitator requires more than just squeezing the bag. A proper mask seal is paramount, achieved with the C-E grip and jaw-thrust maneuver. Visible chest rise confirms air entry, but isn’t always reliable; monitoring tidal volume is preferred.
Studies demonstrate maintaining recommended ventilatory targets during resuscitation is difficult, often exceeding ideal tidal volumes. Utilizing pediatric bags for adults, due to their smaller volumes, can help deliver more appropriate breaths, aligning with guidelines;
Supplemental oxygen is vital, ideally flowing at 15 liters per minute. Consistent rate (10-12 breaths/minute for adults) and avoiding overventilation are key to preventing complications like MVILI and hemodynamic instability. Regular assessment and adjustment are crucial for optimal patient outcomes;
Importance of Supplemental Oxygen
Supplemental oxygen is critically important when using a manual resuscitator, maximizing oxygen delivery to the patient. Gas-powered resuscitators offer a distinct advantage, capable of delivering 100% oxygen, unlike standard manual devices. However, even with manual resuscitators, high-flow oxygen is essential.
Connecting the resuscitator to a 50 psi oxygen source ensures adequate oxygenation. A flow rate of 15 liters per minute is generally recommended to flush the reservoir bag and maintain a high inspired oxygen concentration.
Without sufficient oxygen, the benefits of effective ventilation are diminished. Prioritizing high-flow oxygen alongside proper ventilation technique significantly improves patient outcomes during resuscitation efforts, addressing potential hypoxia and supporting vital organ function.
Potential Complications & Risks
Manual ventilation carries risks like lung injury (MVILI), overventilation causing hemodynamic instability, and esophageal distension due to increased airway pressures.
Manual-Ventilation-Induced Lung Injury (MVILI)
Manual-Ventilation-Induced Lung Injury (MVILI) represents a significant concern during resuscitation efforts utilizing manual resuscitators. This iatrogenic lung damage arises from excessive or forceful ventilation, leading to barotrauma and volutrauma. The concern stems from the potential for hemodynamic changes during manual hyperventilation, which could severely impact patient outcomes and survival rates.
Specifically, the forceful delivery of air can overdistend alveoli, causing rupture and subsequent pneumothorax. Furthermore, high airway pressures can compromise venous return to the heart, reducing cardiac output and overall oxygen delivery. The use of a mask, a common component of manual ventilation, can also expose the patient’s esophagus to increased airway pressure, contributing to gastric inflation and potential aspiration risks. Recognizing and mitigating these risks is crucial for optimizing patient care during emergency ventilation.
Overventilation and its Hemodynamic Effects
Overventilation, a frequent complication during manual resuscitator use, significantly impacts hemodynamics. Excessive ventilation decreases systemic vascular resistance and cardiac output, potentially worsening tissue perfusion. This occurs because hyperventilation leads to hypocapnia – a reduction in carbon dioxide levels – causing cerebral vasoconstriction and decreased blood flow to the brain.
The resulting hemodynamic changes can severely compromise resuscitation efforts, particularly in patients already experiencing shock or compromised cardiovascular function. Authors have expressed concern that these alterations could negatively affect outcomes and survival. Maintaining appropriate ventilation rates and tidal volumes is therefore paramount. Careful monitoring and adherence to current guidelines are essential to avoid the detrimental effects of overventilation and optimize patient stability during manual ventilation.
Esophageal Distension from Increased Airway Pressure
Esophageal distension represents a significant risk associated with manual resuscitator use, particularly when employing a mask. Increased airway pressure during ventilation can inadvertently force air into the esophagus, leading to gastric inflation. This distension not only compromises lung volumes but also triggers a vagal response, potentially causing bradycardia and further hemodynamic instability.
The risk is heightened with improper mask seal or excessive ventilation force. Careful technique, ensuring a tight mask fit and avoiding overly vigorous squeezes of the bag, is crucial. Some forms of manual ventilation, specifically mask ventilation, directly expose the patient’s esophagus to these elevated pressures. Minimizing this risk is vital for preventing complications and optimizing the effectiveness of manual resuscitation efforts.

Current Guidelines and Recommendations
Recent guidelines, like the 2021 NAEMSP statement, advocate for volume-restricted bags for adults and the consistent application of PEEP during ventilation.
NAEMSP Position Statement on Manual Ventilation (2021)
The National Association of EMS Physicians (NAEMSP) released a pivotal position statement in 2021 concerning manual ventilation practices. This statement directly addresses the challenges of maintaining optimal ventilatory targets during resuscitation, acknowledging frequent instances of exceeding recommended tidal volumes. A core recommendation centers on utilizing volume-restricted bags specifically for adult patients.
This shift towards smaller-volume bags, such as pediatric resuscitators for adult use, aims to mitigate the risks associated with overventilation and subsequent complications. The NAEMSP also strongly advocates for the routine application of Positive End-Expiratory Pressure (PEEP) in both adult and pediatric patients undergoing manual ventilation. Implementing PEEP helps maintain alveolar recruitment and improves oxygenation.

Ultimately, the NAEMSP’s guidance seeks to standardize best practices, reduce the incidence of Manual-Ventilation-Induced Lung Injury (MVILI), and enhance patient outcomes during critical care scenarios involving manual resuscitators.
Use of Volume-Restricted Bags for Adults
Employing volume-restricted bags for adult manual ventilation is gaining traction as a strategy to combat overventilation, a common issue during resuscitation efforts. Traditional adult bags often deliver excessive tidal volumes, potentially leading to complications like Manual-Ventilation-Induced Lung Injury (MVILI) and adverse hemodynamic effects. Several studies demonstrate difficulty maintaining recommended ventilation targets with standard bags.
Consequently, utilizing pediatric resuscitator bags for adult patients is increasingly suggested. These bags possess smaller volumes, inherently delivering lower tidal volumes more aligned with established guidelines. This approach directly addresses the NAEMSP’s 2021 position statement advocating for volume restriction.
However, careful consideration is crucial; clinicians must be aware of the reduced bag volume and adjust ventilation rates accordingly to ensure adequate oxygenation and avoid hypoventilation. Proper training and understanding are paramount for successful implementation.
Application of PEEP in Adult and Pediatric Patients
Positive End-Expiratory Pressure (PEEP) application during manual ventilation is increasingly recommended for both adult and pediatric patients, aiming to improve oxygenation and reduce lung injury. PEEP helps maintain alveolar recruitment, preventing collapse during exhalation and enhancing gas exchange. The NAEMSP’s 2021 position statement explicitly supports PEEP utilization in both patient populations.
While traditionally less emphasized in prehospital settings, incorporating PEEP can mitigate the risks associated with manual ventilation, such as atelectasis and MVILI. However, careful titration is essential. Excessive PEEP can compromise venous return and cardiac output, potentially leading to hemodynamic instability.
Clinicians should monitor patient response closely, adjusting PEEP levels based on clinical assessment and, when available, physiological monitoring. Proper training and understanding of PEEP’s physiological effects are crucial for safe and effective application.

Assessment of Ventilation Effectiveness
Effective ventilation assessment requires monitoring tidal volume (VT) and avoiding excessive ventilation, as overinflation can negatively impact patient outcomes during resuscitation.
Monitoring Tidal Volume (VT)
Accurate assessment of ventilation during manual resuscitator use hinges on monitoring tidal volume (VT), the amount of air delivered with each breath. Studies reveal maintaining recommended VT levels during resuscitation is challenging, often exceeding guidelines. This overventilation can lead to complications and negatively affect patient outcomes.
While direct VT measurement requires specialized equipment not always readily available in pre-hospital settings, recognizing the potential for excessive ventilation is crucial. Utilizing a pediatric resuscitator bag for adult patients is a strategy to deliver smaller, more appropriate VT, aligning with recommended guidelines. This approach, encouraged by the NAEMSP position statement, aims to mitigate complications stemming from overinflation.
Clinicians must remain vigilant, understanding that consistent adherence to optimal VT targets is difficult to achieve in dynamic resuscitation scenarios, necessitating careful observation and adjustments.
Avoiding Excessive Ventilation
Excessive ventilation with a manual resuscitator poses significant risks, potentially inducing manual-ventilation-induced lung injury (MVILI) and causing detrimental hemodynamic effects. Hyperventilation can severely impact resuscitation outcomes and survival rates, highlighting the need for careful technique. Maintaining appropriate ventilation rates is paramount, as overinflation exposes the patient’s esophagus to increased airway pressure.
Strategies to mitigate this risk include utilizing volume-restricted bags, particularly for adult patients, as recommended by the NAEMSP. Employing a pediatric bag for adults can also deliver smaller tidal volumes, reducing the likelihood of overventilation. Clinicians should prioritize delivering breaths at an appropriate rate, avoiding rapid or forceful compressions of the reservoir bag.
Continuous assessment and mindful adjustments are essential to prevent the harmful consequences of excessive ventilation during manual resuscitation efforts.